- What is Patient Portal Development?
- What are the Key Features of a Patient Portal?
- How Do You Build a Patient Portal? Development Process Explained
- What are the Benefits of Patient Portal Development?
- How Much Does Patient Portal Development Cost?
- What are the Challenges of Patient Portal Development and How to Overcome Them?
- What Compliance Requirements Apply to Patient Portal Development?
- What is the Future of Patient Portal Development?
- Transform Patient Care With Space-O Technologies
- Frequently Asked Questions about Patient Portal Development
Patient Portal Development: Complete Guide to Features, Cost, and Implementation

Is your healthcare organization still relying on phone calls and paper forms to manage patient communication? You’re not alone – but you’re also falling behind.
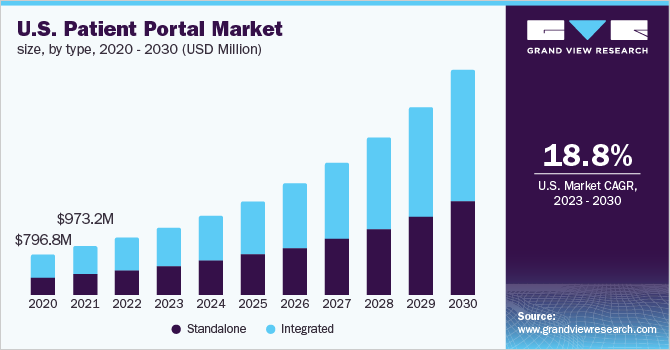
According to Grand View Research, the global patient portal market reached USD 3.92 billion in 2024 and is projected to grow to USD 11.8 billion by 2030, driven by federal mandates and rising patient expectations for digital healthcare access.
This guide breaks down everything you need to know about patient portal development – from core features and development process to costs, compliance requirements, and implementation challenges. Whether you’re a hospital CTO evaluating vendors or a medical practice administrator planning your first portal, you’ll find actionable insights to guide your project.
Looking to build a comprehensive healthcare software development strategy? Patient portals are a critical component of the broader digital health ecosystem.
What is Patient Portal Development?
Patient portal development is the process of building secure, web-based platforms that give patients 24/7 access to their personal health information and enable direct communication with healthcare providers.
Patient portals serve as the patient-facing layer of a healthcare organization’s digital infrastructure. They connect to backend systems like Electronic Health Records (EHR) and practice management software to pull real-time data while maintaining strict security and privacy standards required by PIPEDA.
For Canadian healthcare organizations, patient portal development must account for provincial regulations like PHIPA in Ontario, data residency requirements, and integration with provincial health information systems. Space-O Technologies understands these unique requirements and builds portals that meet both federal and provincial compliance standards.
For healthcare organizations considering healthcare software development solutions, patient portals represent a high-impact starting point that delivers immediate value to both patients and providers.
With a clear understanding of what patient portals are, let’s explore the essential features that make them effective for both patients and providers.
What are the Key Features of a Patient Portal?
Here, we’ll break down the must-have features for patient portal development, organized by priority tier to help you plan your implementation.
1. Health records access and management
Patients securely view and download complete medical histories, including diagnoses, allergies, immunizations, and lab results with reference ranges. Most hospitals now enable clinical notes access directly through portals. Modern portals support sharing records across providers and importing data from external healthcare organizations for coordinated care.
2. Appointment scheduling and reminders
Real-time provider availability lets patients book, reschedule, and cancel visits without phone calls. Automated SMS, email, and push notification reminders significantly reduce no-show rates. Pre-visit form completion and waitlist management for cancellation openings further streamline the scheduling workflow for patients and staff alike.
3. Secure messaging and communication
PIPEDA-compliant two-way messaging eliminates phone tag between patients and care teams. Encrypted message threads support attachments, read receipts, and response time tracking. Intelligent routing directs routine requests to support staff while escalating clinical questions to appropriate providers. After-hours auto-responses guide patients toward emergency resources when needed.
Pro Tip: Implement message triage protocols to prevent provider burnout. Route routine requests (refills, scheduling) to support staff while escalating clinical questions to appropriate providers.
4. Prescription management and refills
Patients view current medications with dosage instructions and request one-click refills sent directly to their preferred pharmacy. Drug interaction alerts and refill reminder notifications improve medication adherence. E-prescribing integration for controlled substances and complete medication history tracking support safer, more efficient prescription management across care teams.
For organizations building comprehensive digital health solutions, prescription management integrates naturally with healthcare app development to enable virtual consultations with prescription capabilities.
5. Billing, payments, and insurance management
Itemized bill viewing, online payment processing, and payment plan setup give patients full financial transparency. Support for credit cards, ACH, and HSA/FSA accounts simplifies transactions. Canadian healthcare organizations benefit from integration with local processors like Moneris and Interac alongside international options for cross-border payment flexibility.
6. Telehealth and virtual visit integration
Patients schedule, join, and manage video consultations through WebRTC directly within the healthcare web platform. Virtual waiting rooms display queue position, while screen sharing enables collaborative review of results. Post-visit summaries are delivered automatically through the portal. Integration with remote monitoring devices extends virtual care beyond scheduled appointments into continuous health tracking.
Space-O Technologies has extensive experience integrating telehealth capabilities into healthcare platforms, ensuring PIPEDA-compliant video consultations that work seamlessly across devices.
Build a Patient Portal Aligned With Clinical and Operational Workflows
Space-O works closely with healthcare teams to ensure portal functionality reflects real-world clinical and administrative processes.
Now that you understand the features, let’s walk through the step-by-step process of building a patient portal from concept to launch.
How Do You Build a Patient Portal? Development Process Explained
Here’s our proven six-phase development process for building secure, compliant patient portals that integrate seamlessly with your existing healthcare systems.
Phase 1: Discovery and requirements gathering
Every successful patient portal development project begins with comprehensive discovery. This phase aligns stakeholders, defines scope, and establishes the compliance framework.
Discovery activities include:
- Stakeholder interviews with clinical staff, administrators, IT, and patient representatives
- Current workflow analysis and pain point identification
- Portal type selection (standalone vs. integrated)
- Feature prioritization using MoSCoW method (Must have, Should have, Could have, Won’t have)
- Compliance roadmap development (PIPEDA, PHIPA, provincial regulations)
- Technology stack selection based on existing infrastructure
- Integration requirements mapping for EHR, billing, and lab systems
Timeline: 2-4 weeks
Deliverables: Requirements document, compliance checklist, technical architecture proposal, project roadmap
Phase 2: Design and prototyping
User experience determines portal adoption. This phase creates intuitive interfaces that work for diverse patient populations while meeting accessibility standards.
Design activities include:
- UX research with patient and provider personas
- Information architecture and user flow mapping
- Wireframes for all major screens and interactions
- High-fidelity UI designs with brand alignment
- Interactive prototypes for stakeholder review
- ADA/WCAG 2.1 AA accessibility planning
- Mobile-responsive design for all screen sizes
Timeline: 3-6 weeks
Deliverables: Wireframes, UI design system, interactive prototype, accessibility compliance plan
Pro Tip: Involve actual patients in usability testing during the design phase. Their feedback often reveals navigation issues and terminology confusion that internal teams miss.
Phase 3: Development and EHR integration
The development phase transforms designs into functional software while building critical integrations with healthcare IT systems.
Development activities include:
- Frontend development using React, Angular, or Vue.js
- Backend API development with Node.js, Python, or .NET
- Database architecture with PIPEDA-compliant encryption
- FHIR R4 and HL7 v2/v3 integration connectors for EHR systems
- Security implementation: AES-256 encryption, MFA, role-based access control (RBAC)
- Mobile app development (native iOS/Android or cross-platform with React Native/Flutter)
- Payment gateway integration
- Notification system setup (SMS, email, push)
Timeline: 8-20 weeks, depending on complexity
Deliverables: Functional portal application, API documentation, integration specifications
For organizations seeking specialized expertise, Space-O Technologies’ team includes developers experienced in FHIR API integration, healthcare security protocols, and EHR connectivity with major systems, including Epic, Cerner, and Athenahealth.
Phase 4: Testing and compliance validation
Rigorous testing ensures the portal works correctly, securely, and in compliance with healthcare regulations before patient data enters the system.
Testing activities include:
- Unit testing for individual components
- Integration testing for EHR and third-party connections
- Security penetration testing by qualified assessors
- PIPEDA compliance validation and documentation
- Performance and load testing under expected patient volumes
- Usability testing with representative patient groups
- Accessibility testing with assistive technologies
- Cross-browser and cross-device compatibility testing
Timeline: 3-6 weeks
Deliverables: Test reports, security assessment, compliance documentation, bug resolution
Phase 5: Deployment and training
Successful deployment requires careful planning, staff preparation, and patient communication to drive adoption from day one.
Deployment activities include:
- Production environment setup with monitoring and alerting
- Data migration from legacy systems (if applicable)
- Staff training on portal administration and patient support
- Patient onboarding materials: quick-start guides, video tutorials, FAQ
- Phased rollout strategy (pilot group before full launch)
- Go-live support with a dedicated response team
- Patient communication campaign to drive registration
Timeline: 2-4 weeks
Deliverables: Production deployment, training materials, patient communication kit, support protocols
Phase 6: Ongoing maintenance and support
Patient portal development doesn’t end at launch. Continuous maintenance ensures security, compliance, and evolving functionality.
Ongoing activities include:
- Bug fixes and performance optimization
- Security patches and vulnerability remediation
- Feature enhancements based on user feedback
- Compliance updates for regulatory changes (PIPEDA Security Rule updates, provincial requirements)
- EHR integration maintenance as vendor APIs evolve
- 24/7 technical support for critical issues
- Regular backup and disaster recovery testing
Annual Cost: 15-20% of original development investment
Space-O Technologies provides comprehensive post-launch support, including 3 months of free maintenance, ensuring your portal remains secure, compliant, and optimized for patient engagement.
With the development process clear, let’s examine the tangible benefits patient portals deliver to healthcare organizations.
What are the Benefits of Patient Portal Development?
This section explores how patient portals benefit healthcare organizations, from operational efficiency to improved patient outcomes and cost savings.
1. Enhanced patient engagement and satisfaction
Patient portals give individuals 24/7 access to health records, test results, and care plans without office hour constraints. Faster communication eliminates long hold times for routine questions. Patients manage appointments, prescription refills, and billing from any device. Research confirms provider endorsement remains the single most effective driver of portal adoption.
2. Reduced administrative burden and costs
Portals automate routine tasks like appointment scheduling, refill requests, and billing inquiries that consume significant staff time. Automated reminders alone reduce no-show rates by roughly 25-35%. Pre-visit digital form completion accelerates patient intake. Streamlined referral coordination and reduced paper mailing costs allow healthcare organizations to redirect resources toward direct patient care.
3. Improved clinical outcomes
Faster test result delivery lets patients access findings within hours instead of waiting for callbacks. Refill reminders and digital medication lists improve adherence across treatment plans. Secure messaging enables earlier symptom identification and timely provider intervention. Better chronic disease management follows when patients actively engage with their health data through portal access.
4. Healthcare regulatory compliance
Patient portals fulfill 21st Century Cures Act requirements for API-based data access and demonstrate a good faith effort against information blocking rules. They support PIPEDA electronic access rights and Promoting Interoperability measures. Comprehensive audit trails document all patient data access and communications. Organizations without adequate portal functionality face increasing regulatory scrutiny and potential penalties.
5. Competitive advantage in healthcare delivery
Patients now expect digital access comparable to banking and retail experiences. Portals attract younger demographics who evaluate providers based on digital capabilities before scheduling appointments. Supporting value-based care models that reward engagement and outcomes positions organizations for future innovation. Portals provide the foundation for integrating AI, remote monitoring, and personalized care.
Healthcare organizations investing in healthcare software modernization recognize that patient portals are essential infrastructure for competing in the digital health era.
Understanding the benefits naturally leads to a critical question – how much does patient portal development actually cost?
How Much Does Patient Portal Development Cost?
Let’s break down patient portal development costs by complexity tier, helping you budget accurately for your healthcare organization’s needs.
1. Cost breakdown based on types
| Tier | Cost Range (CAD) | Key Features | Best For | Timeline | Team Size |
|---|---|---|---|---|---|
| Basic | $40,000–$135,000 | Patient registration/secure login (MFA), health records view/download, appointment scheduling/reminders, secure messaging, basic billing/payment, mobile-responsive design | Small practices (5-20 providers), specialty clinics, urgent care, and dental | 2-3 months | 2-3 developers, 1 UI/UX, 1 QA, 1 PM |
| Mid-range | $135,000–$200,000 | All basic + EHR integration (Epic/Cerner/etc), telehealth video, e-prescribing, lab/imaging results/trending, education library, admin analytics, native iOS/Android apps | Medium practices, regional clinics, community health centers, multi-specialty groups | 3-6 months | 4-6 specialists (incl. integration/mobile devs) |
| Enterprise | $200,000–$450,000+ | All mid-range + multi-facility support, AI chatbots, advanced analytics/population health, wearable/remote monitoring, custom workflows, multi-language, white-label, advanced APIs | Hospitals, health systems, academic centers, multi-state networks | 6-12+ months | 8-12+ specialists (incl. AI/ML, integration architects, compliance) |
2. Key factors that influence development cost
Several variables can significantly impact your patient portal development budget:
EHR integration complexity: Each EHR system requires custom integration work. Epic integration differs substantially from Cerner or Athenahealth. Budget $25,000–$70,000+ per major system integration.
Compliance requirements: Add PIPEDA for Canadian operations, GDPR for European patients, or state-specific requirements, and compliance overhead increases.
Platform scope: Web-only development costs less than web plus native iOS and Android apps. Cross-platform frameworks (React Native, Flutter) offer cost savings of 30-40% compared to separate native development.
Customization level: Off-the-shelf templates cost less but limit differentiation. Custom UI/UX design and unique workflows add 30-50% to base development costs.
Development team location: North American development firms ($135–$275/hour) cost more than Eastern European firms ($70–$110/hour) or Offshore firms in regions like India or Southeast Asia ($35–$70/hour). Space-O Technologies offers competitive rates with the communication advantages of a Canadian partner.
Control Patient Portal Costs Without Compromising Compliance
Space-O helps prioritize essential features while accounting for PIPEDA requirements and long-term operational needs.
With budget considerations in mind, let’s address the common challenges organizations face during patient portal development and how to overcome them.
What are the Challenges of Patient Portal Development and How to Overcome Them?
Patient portal development comes with significant challenges – from data security to user adoption. Here’s how to navigate these obstacles successfully.
1. Data privacy and security concerns
The Challenge: Healthcare data breaches are among the most costly across all industries, averaging $4.4 million (USD) per incident, according to this IBM report. Patient portals expand the attack surface by creating new access points to sensitive health information.
How to Overcome It:
- Implement AES-256 encryption for data at rest and TLS 1.3 for data in transit
- Require multi-factor authentication (MFA) for all patient logins
- Deploy role-based access control (RBAC) to limit data exposure
- Conduct regular penetration testing by qualified security assessors
- Establish 24-hour breach notification protocols
- Monitor for suspicious access patterns with automated alerting
Security must be built into the architecture from day one – retrofitting security into an existing portal is significantly more expensive and less effective.
2. EHR integration complexity
The Challenge: With 40+ EHR systems in the market, each with different APIs, data models, and compatibility requirements, integration is often the most technically complex aspect of patient portal development.
How to Overcome It:
- Prioritize FHIR R4 APIs as the modern interoperability standard mandated by the 21st Century Cures Act
- Use interface engines like Mirth Connect, Rhapsody, or SmileCDR for data translation
- Partner with developers experienced in your specific EHR system (Epic, Cerner, Athenahealth, MEDITECH)
- Plan for ongoing integration maintenance as EHR vendors update their APIs
- Document all integration specifications for future troubleshooting
Space-O Technologies’s development team has hands-on experience integrating with major EHR platforms, understanding the nuances of each vendor’s approach to data exchange.
3. Low patient adoption rates
The Challenge: Despite 90%+ of healthcare organizations offering patient portals, only 30-50% of patients actively use portal features. Simply building a portal doesn’t guarantee engagement.
How to Overcome It:
- Provider encouragement – patients whose providers actively recommend portal use show significantly higher adoption
- Intuitive UX design – prioritize simplicity over feature richness initially
- Patient education campaigns – explain benefits and provide setup assistance
- Multi-language support – remove language barriers for diverse patient populations
- Mobile-first design – 57% of patients now use apps to access records
- Simplified registration – reduce friction in the initial signup process
Pro Tip: Track portal adoption metrics by demographic and provider. This data reveals which patient populations need additional outreach and which providers are most effective at encouraging portal use.
4. Provider resistance and workflow disruption
The Challenge: Clinical staff may resist patient portals due to increased message volume, workflow changes, and concerns about technology replacing clinical judgment. Provider burnout from portal messages is a growing concern.
How to Overcome It:
- Involve clinicians in the design process from discovery through testing
- Integrate portal alerts into existing EHR workflows rather than creating separate systems
- Establish message response protocols with clear expectations and routing rules
- Route routine requests (refills, scheduling) to support staff
- Provide training that demonstrates how portals reduce – not increase – overall workload
- Monitor message volumes and adjust staffing accordingly
5. Regulatory compliance burden
The Challenge: Navigating PIPEDA, provincial regulations, and 21st Century Cures Act requirements creates significant complexity, especially for organizations operating across multiple jurisdictions.
How to Overcome It:
- Build compliance into architecture from the start rather than adding it later
- Engage compliance specialists during the discovery phase
- Document all compliance measures for audit readiness
- Conduct regular compliance audits and update practices as regulations evolve
- Partner with development teams who understand healthcare regulations
For Canadian healthcare organizations, compliance extends beyond federal PIPEDA to include provincial requirements like PHIPA (Ontario), BC PIPA, and Alberta PIPA. Organizations seeking help can outsource healthcare software development to partners with proven compliance expertise.
6. Legacy system compatibility
The Challenge: Many healthcare organizations operate decades-old systems lacking modern integration capabilities. Connecting patient portals to legacy infrastructure requires custom development or wholesale system replacement.
How to Overcome It:
- Assess legacy system capabilities honestly during discovery
- Use middleware and interface engines to bridge technology gaps
- Prioritize phased implementation starting with the highest-value, easiest-to-integrate features
- Plan a gradual migration rather than a big-bang replacement
- Budget for custom adapter development where standard integrations don’t exist
Overcoming these challenges requires understanding the regulatory landscape – let’s explore the compliance requirements for patient portal development.
What Compliance Requirements Apply to Patient Portal Development?
This section covers the regulatory landscape for patient portals, including PIPEDA, and the latest 2026 security updates healthcare organizations must address.
1. Canadian compliance: PIPEDA and provincial regulations
Canadian healthcare organizations face a layered compliance landscape that differs significantly from the U.S. approach.
PIPEDA (Personal Information Protection and Electronic Documents Act):
- Consent-based model requiring opt-in for personal information collection
- 10 fair information principles governing data handling
- Breach reporting to the Office of the Privacy Commissioner
- Applies to all provinces without equivalent provincial legislation
Provincial health information laws:
- PHIPA (Ontario) – specific rules for personal health information, consent requirements, and access rights
- BC PIPA – prohibits the storage of personal information outside Canada unless consent is given
- Alberta PIPA – similar to PIPEDA with provincial enforcement
- Quebec Law 25 – mandatory privacy officers, 72-hour breach reporting, penalties up to $25M or 4% global revenue
Key differences from U.S. (HIPAA):
- Canada uses an opt-in consent vs. the U.S. opt-out approach
- PIPEDA covers all personal information, not just health data
- Some provinces prohibit data storage outside Canada, even with encryption
- Penalty structures increasingly rival GDPR levels
Space-O Technologies builds patient portals with Canadian compliance requirements integrated from the architecture level, ensuring data residency, consent management, and provincial requirements are properly addressed.
2. 21st Century Cures Act and information blocking
The 21st Century Cures Act fundamentally changed patient data access requirements in the United States, with implications for any organization serving U.S. patients.
Key requirements:
- Patient API access – healthcare organizations must provide patients with electronic access to their health data
- Information blocking prohibition – organizations cannot prevent or discourage access to electronic health information
- FHIR-based data exchange – FHIR R4 is the required standard for patient-facing APIs
- USCDI compliance – United States Core Data for Interoperability defines minimum data sets
Organizations without adequate patient portal functionality may face regulatory action under information blocking rules. The ONC has enforcement authority and can impose civil monetary penalties.
Compliance requirements lead us to another important question: where is patient portal technology headed to help future-proof your investment?
What is the Future of Patient Portal Development?
Here’s what’s next for patient portals – from AI-powered features to wearable integration and the technologies shaping healthcare’s digital future.
1. AI and machine learning integration
Artificial intelligence transforms patient portals into proactive health companions. AI-powered chatbots deliver 24/7 support using natural language processing for triage, symptom checking, and appointment scheduling.
Predictive health analytics identify patients at risk for readmission or disease progression. Personalized care recommendations are then adapted to individual health profiles, conditions, and treatment preferences.
Organizations already investing in predictive analytics in healthcare can extend those capabilities into patient-facing portal features.
2. Wearable and remote monitoring
Patient portals now integrate data from consumer wearables like Apple Watch and Fitbit alongside clinical-grade devices, including continuous glucose monitors and blood pressure cuffs.
Real-time alerting notifies care teams when patient readings exceed clinical thresholds, aligning with the broader future of healthcare technology. Trend visualization helps both patients and providers identify meaningful patterns in longitudinal health data.
3. Mobile-first and voice-enabled access
Patient portal access is shifting to mobile devices as the primary interface. Native apps now support voice navigation through Alexa, Google Assistant, and Siri for hands-free interaction.
Biometric authentication using fingerprint and facial recognition enables seamless, secure login. Offline capabilities ensure patients have access to critical health information even without reliable connectivity.
Improve Patient Experience Through Intuitive Portal Design
Space-O prioritizes usability, accessibility, and clear information structure to help patients navigate healthcare tasks with confidence.
With a clear understanding of patient portal development – from features and costs to challenges and future trends – let’s summarize how to move forward with your project.
Transform Patient Care With Space-O Technologies
Patient portal development has evolved from a competitive differentiator to an essential healthcare infrastructure. With patient expectations shifting toward digital access and regulations requiring electronic health information sharing, organizations without robust patient portals face both competitive disadvantage and regulatory risk.
Since 2018, Space-O Technologies has been offering software development services to healthcare organizations across North America. Our team understands the unique requirements of Canadian healthcare – from PIPEDA and PHIPA compliance to integration with provincial health systems.
We deliver custom patient portal solutions tailored to your clinical workflows and patient population, with PIPEDA compliance built into every implementation. Our team integrates seamlessly with leading EHR systems such as Epic, Cerner, Athenahealth, and MEDITECH, while maintaining transparent pricing with no hidden costs.
Ready to build a patient portal that transforms your healthcare delivery? at Space-O Technologies helps healthcare organizations develop secure, compliant patient portals that improve patient engagement, reduce administrative burden, and position you for the future of digital health.
Frequently Asked Questions about Patient Portal Development
How long does it take to develop a patient portal?
Patient portal development timelines vary by complexity. Basic portals with essential features take 2-4 months. Mid-range portals with EHR integration and telehealth require 4-6 months. Enterprise portals for health systems with multiple facilities and advanced features take 6-12+ months. Timeline depends on integration complexity, customization requirements, and regulatory scope.
What EHR systems can patient portals integrate with?
Modern patient portals can integrate with virtually any EHR system that supports FHIR R4 or HL7 standards. Common integrations include Epic (MyChart), Oracle Health (Cerner), Athenahealth, MEDITECH, eClinicalWorks, NextGen Healthcare, and Allscripts. Each system requires specific integration work, and costs vary based on API complexity and data requirements.
Is HIPAA compliance required for patient portals?
Yes, HIPAA compliance is mandatory for any patient portal that handles Protected Health Information (PHI) for U.S. patients. This includes implementing encryption, access controls, audit logging, and breach notification procedures. Canadian portals must also comply with PIPEDA and applicable provincial regulations like PHIPA in Ontario.
Can patient portals work on mobile devices?
Absolutely. Modern patient portal development prioritizes mobile access through responsive web design and native iOS/Android applications. In 2024, 57% of patients used mobile apps to access their health records. Mobile portals should include biometric login, push notifications, and offline access to critical information.
What is the ROI of patient portal development?
Patient portal ROI comes from multiple sources: reduced administrative costs (fewer phone calls, automated scheduling), decreased no-show rates (up to 28% reduction with automated reminders), faster payment collection, improved patient satisfaction scores, and regulatory compliance. Most organizations achieve positive ROI within 12-24 months of implementation.
How do you ensure patient portal security?
Patient portal security requires multiple layers: AES-256 encryption for data at rest, TLS 1.3 for data in transit, multi-factor authentication, role-based access controls, regular penetration testing, continuous monitoring for suspicious activity, and documented incident response procedures. Security must be built into the architecture from day one, not added after development.

All our projects are secured by NDA
100% Secure. Zero Spam
*All your data will remain strictly confidential.
Trusted by


Bashar Anabtawi
Canada
“I was mostly happy with the high level of experience and professionalism of the various teams that worked on my project. Not only they clearly understood my exact technical requirements but even suggested better ways in doing them. The Communication tools that were used were excellent and easy. And finally and most importantly, the interaction, follow up and support from the top management was great. Space-O not delivered a high quality product but exceeded my expectations! I would definitely hire them again for future jobs!”

Canada Office
2 County Court Blvd., Suite 400,
Brampton, Ontario L6W 3W8
Phone: +1 (623) 335-2152
Email: sales@spaceo.ca

